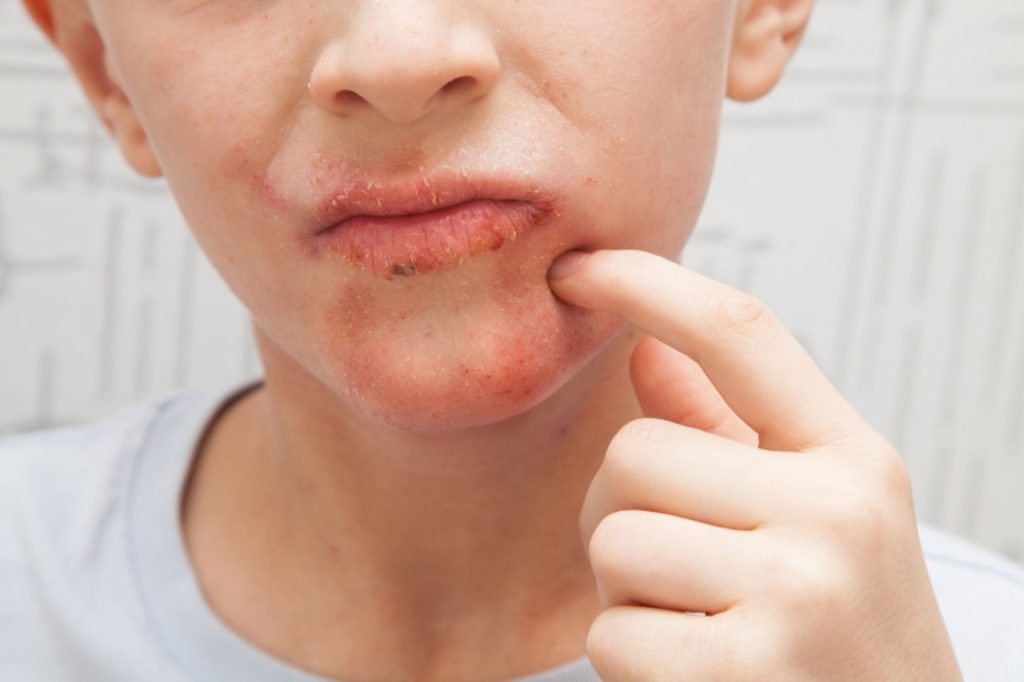
The Impetigo infection begins innocuously as small red sores but quickly evolves into painful, itchy blisters that can dramatically affect a child’s comfort and quality of life. If not treated promptly, impetigo can lead to more severe complications, including scarring and the potential for deeper infections that can spread to other parts of the body.
The ease with which impetigo spreads among children means a single case can quickly become an outbreak, disrupting educational environments and causing widespread concern among parents and educators. That’s why it’s important for parents and caregivers to be able to recognise the signs of impetigo and take appropriate steps to manage the infection effectively.
Identifying Impetigo in Children
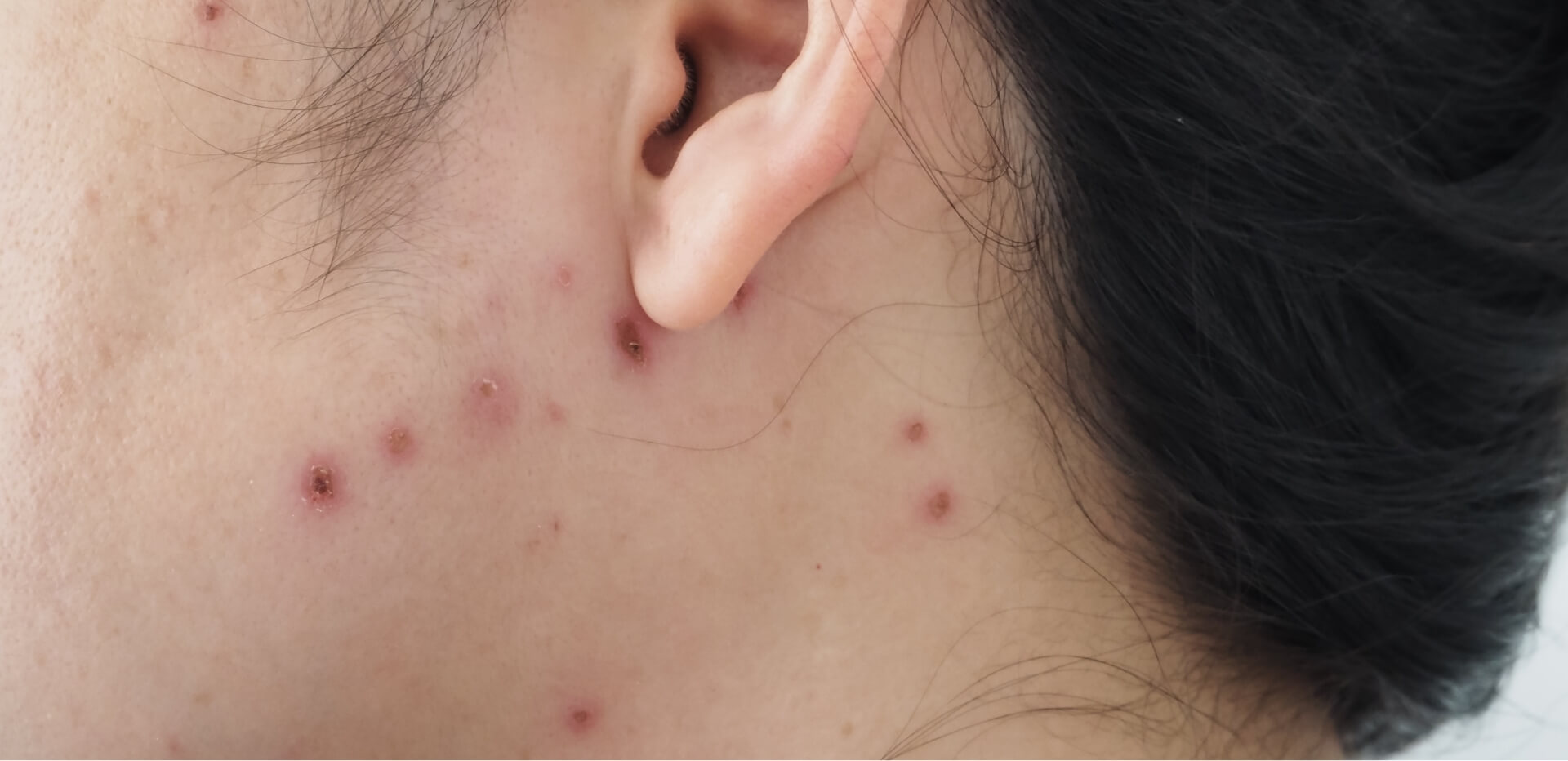
The first step in dealing with impetigo is to be able to identify the condition accurately. Impetigo typically presents as red sores or blisters that rupture and become coated with a yellowish-brown crust. These sores can appear anywhere on the body, but they are most commonly found on the face, particularly around the nose and mouth.
Other signs and symptoms of impetigo may include:
- Itching or pain in the affected areas
- Swollen lymph nodes near the infection site
- Fever (in more severe cases)
It’s important to note that the appearance of impetigo can sometimes be confused with other skin conditions, such as eczema or ringworm. If you’re unsure about the diagnosis, it’s always best to consult our pharmacists.
Causes and Risk Factors
Impetigo is caused by bacterial infection, usually by Staphylococcus aureus or Streptococcus pyogenes. These bacteria can enter the body through cuts, scratches or insect bites or they can spread from person to person through direct contact or shared towels, clothing or other personal items.
Children are particularly susceptible to impetigo due to their tendency to play closely with others, share toys and personal items and their underdeveloped hygiene habits. Other risk factors that can increase the likelihood of developing impetigo include:
- Warm, humid weather (which promotes bacterial growth)
- Crowded living conditions
- Poor personal hygiene
- Compromised immune system
Effective Treatment Options
Once impetigo has been diagnosed, prompt treatment is essential to prevent the spread of the infection and promote healing. The specific treatment approach will depend on the severity of the infection and the age of the child.
Topical Antibiotics
For mild cases of impetigo, topical antibiotic creams or ointments are often prescribed. These medications, such as mupirocin or retapamulin, can help eliminate bacterial infection and promote healing of the sores. Topical antibiotics are typically applied two to three times a day for about a week.
Oral Antibiotics
In more severe cases or if the infection has spread to larger areas of the body, oral antibiotics may be necessary. Common antibiotic choices for impetigo include cephalexin, dicloxacillin or amoxicillin-clavulanate. These medications are typically taken for seven to ten days to ensure complete resolution of the infection.
Home Care and Hygiene
In addition to antibiotic treatment, proper home care and hygiene practices are essential for managing impetigo effectively. Here are some important steps to follow at home for impetigo:
- Keep the affected areas clean and dry: Gently wash the sores with warm water and mild soap and pat them dry with a clean towel.
- Avoid scratching or picking at the sores: This can delay healing and increase the risk of spreading the infection.
- Cover the sores: Use clean bandages or dressings to cover the affected areas, especially when the child is at school or in other public settings.
- Practice good hand hygiene: Encourage frequent handwashing with soap and water, especially after touching the sores or handling any dressings.
- Avoid sharing personal items: Discourage the sharing of towels, clothing or other personal items until the infection has cleared.
- Disinfect surfaces and toys: Regularly clean and disinfect surfaces, toys and other items that the child has come into contact with.
Preventing Impetigo Recurrence and Spread
Even after successful treatment, it’s important to take steps to prevent the recurrence of impetigo and reduce the risk of spreading the infection to others. Here are some preventive measures to consider:
- Practice good hygiene: Encourage regular handwashing, bathing and proper hygiene habits to minimise the risk of bacterial transmission.
- Treat underlying conditions: If the child has a condition like eczema or diabetes that increases the risk of impetigo, ensure proper management and treatment of the underlying condition.
- Avoid sharing personal items: Discourage the sharing of towels, clothing or other personal items, especially during an active infection.
- Keep cuts and scratches clean: Promptly clean and cover any cuts, scratches or insect bites to prevent bacterial entry.
- Stay home when needed: If a child has an active impetigo infection, consider keeping them home from school or daycare until the sores have started to heal and they have been on antibiotics for at least 24 hours.
Schedule Your Child’s Impetigo Consultation
By being able to recognise the signs of impetigo, seeking prompt medical attention and following recommended treatment and hygiene practices, parents and caregivers can effectively manage this contagious skin infection in children. With proper care and preventive measures, impetigo can be resolved without significant complications and the risk of recurrence and spread can be minimised.
If your child is showing signs of impetigo or you have concerns about skin infections, book an appointment with Touchwood Pharmacy today for expert care and treatment. Our friendly pharmacists are ready to provide the guidance and support your child needs without visiting the GP. Contact us to ensure your child’s health and peace of mind.